Dupuytren's Contracture: When Your Fingers Won't Straighten
Author
Mr. Murali Bhat
Published On
22 September 2025
What Is Dupuytren’s Contracture?
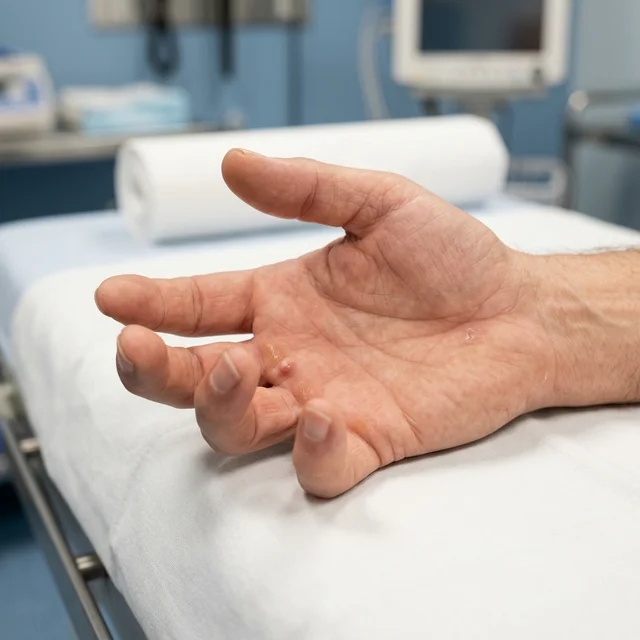
Dupuytren’s contracture (also known as Dupuytren’s disease) is a progressive condition affecting the palmar fascia — the thick layer of tissue that lies beneath the skin of the palm and fingers. Over time, this tissue thickens and forms firm nodules and cords that gradually pull one or more fingers into a bent (flexed) position.
The condition was first described by the French surgeon Baron Guillaume Dupuytren in 1831, and it remains one of the most common hand conditions seen in clinical practice. While rarely painful, the functional impact can be profound — patients often find themselves unable to lay their hand flat on a table, shake hands comfortably, put on gloves, or reach into their pockets.
Who Develops Dupuytren’s?
Dupuytren’s contracture has a strong genetic component and is significantly more prevalent in people of Northern European descent. Key risk factors include:
- Age — The condition is most common in people over 50, though it can present earlier with more aggressive disease.
- Gender — Men are affected approximately six times more often than women, and tend to develop the condition at an earlier age.
- Family history — If a parent or sibling has Dupuytren’s disease, your risk is substantially increased. Multiple genes are thought to be involved.
- Smoking and alcohol consumption — Both are associated with a higher incidence and more aggressive disease progression.
- Diabetes — Approximately 5–20% of diabetic patients develop Dupuytren’s contracture, although it tends to follow a milder course.
- Epilepsy — There is a well-documented association, possibly related to long-term use of anti-epileptic medications.
It is important to understand that Dupuytren’s is not caused by manual labour or repetitive hand use, despite common misconceptions to the contrary.
How Does the Disease Progress?
Dupuytren’s contracture typically progresses through three recognisable stages:
Stage 1: Nodule Formation
The earliest sign is the appearance of one or more firm nodules in the palm, most commonly at the base of the ring or little finger. These nodules sit within the palmar fascia and may be tender initially, though the tenderness usually settles. At this stage, finger movement is usually unaffected.
Stage 2: Cord Development
Over months to years, the nodules mature and coalesce into thick cords of fibrous tissue. These cords extend from the palm into the affected fingers along the line of the tendons, though importantly, they are not part of the tendons themselves. The finger may begin to show a fixed flexion deformity — typically first noticed when the patient cannot fully straighten the affected digit.
Stage 3: Established Contracture
The cords progressively shorten and tighten, pulling the affected fingers into a permanently bent position. The metacarpophalangeal (MCP) joints and proximal interphalangeal (PIP) joints are most commonly involved. In advanced cases, the finger may be drawn so far into the palm that hygiene becomes a concern, and the overlying skin can develop maceration and infection.
The rate of progression varies enormously between individuals. Some patients experience slow, gradual progression over many years, while others — particularly those with a strong family history or early onset — may develop significant contracture within months.
The “Tabletop Test”
A simple and widely used screening tool is the tabletop test: place your hand flat on a table with the palm facing down. If you cannot flatten all your fingers against the table surface, this suggests a contracture of 30 degrees or more — the commonly accepted threshold at which surgical intervention should be considered.
Treatment Options
Treatment is recommended when the contracture interferes with hand function. The optimal timing and approach depend on the degree of contracture, which joints are involved, and the patient’s individual circumstances.
Non-Surgical Options
Collagenase Injection (Xiapex)
A relatively recent non-surgical option involves injecting an enzyme called collagenase clostridium histolyticum directly into the Dupuytren’s cord. The enzyme breaks down the collagen within the cord over 24–48 hours. The patient then returns for a gentle manipulation procedure, during which the weakened cord is snapped to restore finger extension.
Advantages: No incision required. Performed as an outpatient procedure. Faster recovery compared to surgery.
Limitations: Recurrence rates are higher than surgery. Not suitable for all cord patterns, particularly when the cord wraps around neurovascular structures. Availability may be limited.
Needle Fasciotomy (Percutaneous Needle Aponeurotomy)
Using a fine needle inserted through the skin, the Dupuytren’s cord is divided at multiple points. This is performed under local anaesthesia and requires no formal incision.
Advantages: Minimal recovery time. Can be repeated if the disease recurs.
Limitations: Higher recurrence rates compared to open surgery. Risk of nerve or tendon injury, especially in the fingers where these structures lie close to the skin surface.
Surgical Treatment
Fasciectomy
Open surgical fasciectomy remains the gold standard treatment for significant Dupuytren’s contracture. The procedure involves:
- A carefully designed incision in the palm and/or finger — often using a Bruner zigzag pattern to minimise scar contracture.
- Meticulous dissection and excision of the diseased fascia, carefully preserving the digital nerves and arteries that often become encased within the Dupuytren’s tissue.
- Release of the contracted joints to restore extension.
- Skin closure — in some cases, a small skin graft or local flap may be necessary if the overlying skin is severely contracted.
The operation is typically performed under regional anaesthesia (an arm block) as a day-case procedure. A qualified consultant anaesthetist provides the anaesthesia, ensuring patient comfort throughout.
Recovery timeline:
- A bulky dressing is applied for the first few days, then replaced with lighter dressings.
- Sutures are removed at 10–14 days.
- A custom-made night extension splint is fabricated by a specialist hand therapist and worn for approximately 3 months to maintain the correction.
- A structured hand therapy programme guides patients through progressive exercises to restore movement and grip strength.
- Most patients can return to desk work within 2–3 weeks and manual work within 6–8 weeks.
Dermofasciectomy
For recurrent disease or particularly aggressive Dupuytren’s, a dermofasciectomy may be recommended. This involves excision of the diseased fascia along with the overlying skin, which is replaced with a full-thickness skin graft — usually harvested from the inner arm. This technique has the lowest recurrence rate of all available treatments.
Living with Dupuytren’s: What to Expect
Dupuytren’s disease is a chronic condition, and patients should be aware that:
- Recurrence is possible with any treatment method. Regular follow-up allows early detection and timely intervention.
- The disease may affect the other hand over time — bilateral involvement occurs in approximately 50% of patients.
- Early presentation to a specialist ensures a full range of treatment options remain available. Once contracture becomes severe and longstanding, the results of any intervention are less predictable.
When to Seek a Specialist Assessment
We recommend consulting a hand specialist if you notice:
- A firm lump or nodule in the palm of your hand.
- Difficulty fully straightening one or more fingers.
- Progressive bending of a finger that is affecting your ability to grip, shake hands, or perform daily tasks.
- You have a strong family history of Dupuytren’s disease and are noticing early changes.
Early assessment does not necessarily mean immediate treatment — in many cases, monitoring is the appropriate first step. However, establishing a baseline and understanding your individual disease pattern allows for well-timed intervention when needed.
Mr. Murali Bhat is a Consultant Orthopaedic Surgeon specialising in hand, wrist, and upper limb conditions. He practises at Kings Oak Hospital and The Cavell Hospital in Enfield, North London.